 
Patients with symptoms and signs of CRAO must be referred immediately to an ophthalmologist because irreversible damage occurs in as little as 100 minutes of occlusion. Referral to an ophthalmologist within 24 hours Normal conjunctiva and cornea normal pupil pale, detached retina Normal to peripheral or central vision loss absence of pain increasing floaters unilateral photopsia metamorphopsia 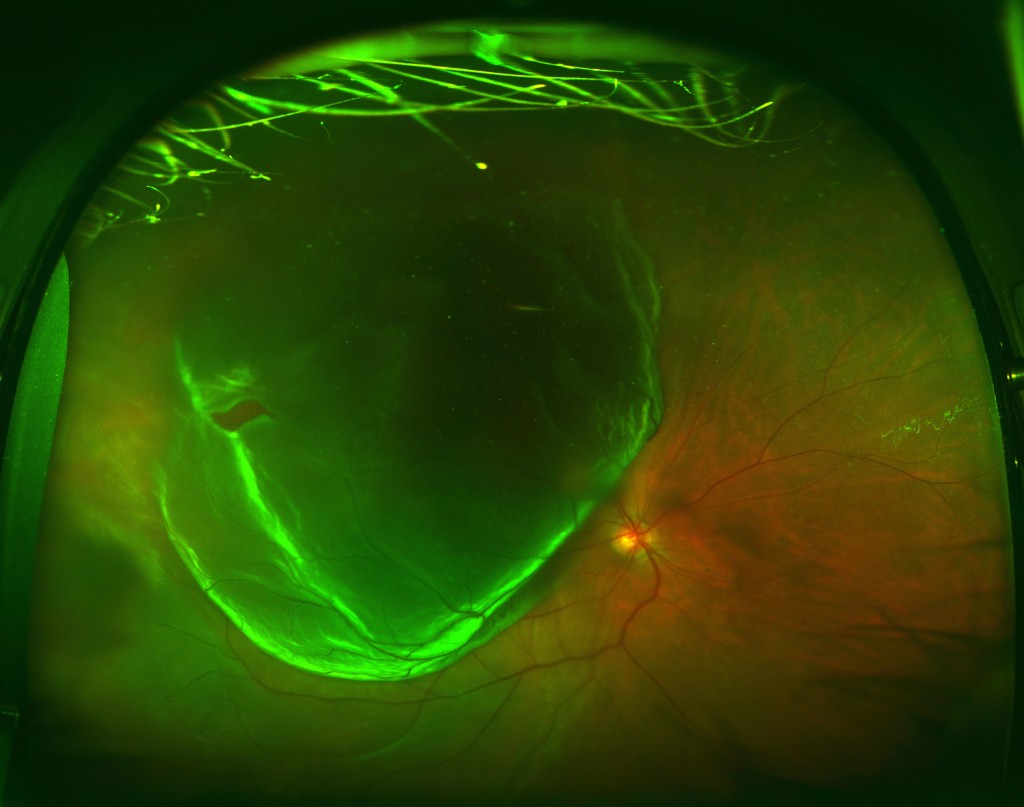
Lowering IOP with acetazolamide 500 mg orally once and one drop each of 0.5% timolol maleate (Timoptic), 1% apraclonidine (Iopidine), and 2% pilocarpine (Isopto Carpine) one minute apart and repeated three times at five-minute intervals Mid-dilated and sluggish pupil normal or hazy cornea shallow anterior chamber Lowering IOP with mannitol (Osmitrol) 0.25 to 2.0 g per kg IV once, acetazolamide (Diamox *) 500 mg IV or orally once, carbogen inhalation, administering oral nitrates, or by laying the patient on his or her backĪcute onset of severe pain blurred vision frontal headache halos around lights increased IOP red eye/conjunctiva Interrupted columns of blood within the retinal vessels (sometimes referred to as “boxcarring”) and attenuation of retinal arteries cherry-red spot at the fovea pale fundus pupil may be dilated and react poorly to light Scheduled analgesia and antiemetics update tetanus immunizationĬornea may have minor epithelial damage or be opaque moderate to severe pain blurred vision reflex blepharospasm photophobia sensation of a foreign body red eye/conjunctivaįindings depend on the severity corneal and scleral melting may occur if injury is severeĮye irrigation with normal saline or lactated Ringer's solution until pH is normalĬontinue eye wash on way to the emergency department or an ophthalmologistĬlear cornea amaurosis fugax (transient, painless unilateral vision loss) or permanent vision loss red eye/conjunctiva Normal or damaged cornea moderate to severe pain normal or decreased vision hyphema red eye/subconjunctival hemorrhage in the area 360 degrees around the corneaĭecreased anterior chamber depth relative to uninjured eye irregular or deviated pupil toward the direction of injury positive Seidel test Unilateral vision loss with Marcus Gunn's pupillary phenomenon *ĭefective pupillary response indicates optic nerve dysfunction or retinal detachment unilateral loss of vision without Marcus Gunn's pupillary phenomenon indicates that the lesion is somewhere other than on the optic nerve or retina Pupillary reflex visual field testing (i.e., the confrontation visual field examination) abnormalityĬentral retinal artery occlusion retinal detachment retinal hemorrhage Orbit and cheek deformity tenderness over the supraorbital ridge or frontal bone Optic nerve (i.e., afferent nerve) dysfunction on one side 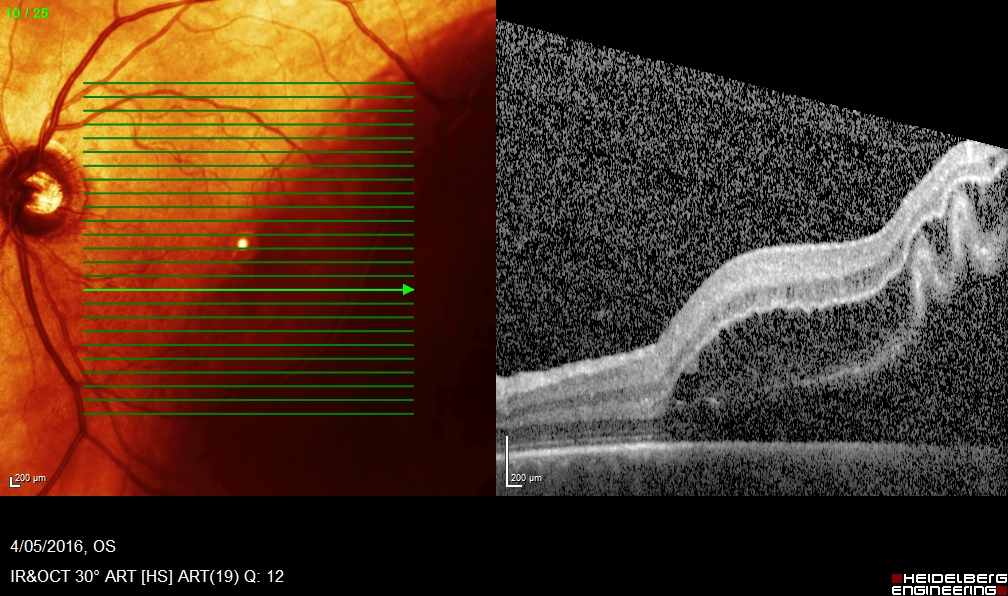
Intact contralateral direct reflex and ipsilateral consensual reflex loss of contralateral consensual reflex and ipsilateral direct reflex Oculomotor nerve (i.e., efferent nerve) dysfunction on one side 
Intact contralateral direct reflex and contralateral consensual reflex loss of ipsilateral consensual reflex and ipsilateral direct reflex Use of an eye shield is required in patients with a ruptured globe to protect the injured eye and preserve the patient's vision.ĭiplopia dysconjugate gaze (i.e., both eyes cannot fix to an object at the same time) ptosisĬranial nerves III, IV, or VI palsy extraocular muscle paresis or paralysisĪssociated globe perforation damage to the lacrimal drainage system or levator muscle After a chemical burn, thorough eye washing for at least 30 minutes or until the pH of the eye is within physiologic range is critical to prevent further damage. Ocular injury from high-velocity trauma or from chemicals may be easily misdiagnosed. Confrontation visual field examination, pupillary examination, and direct ophthalmoscopy of both eyes also should be performed. All patients with eye problems should be tested for visual acuity and ocular movements. Careful eye examination and simple tests can help primary care physicians make decisions about appropriate treatment and referral. All ocular emergencies, including a penetrating globe injury, retinal detachment, central retinal artery occlusion, acute angle-closure glaucoma, and chemical burns, should be referred immediately to the emergency department or an ophthalmologist. Prompt recognition and appropriate treatment of ocular emergencies are essential in the primary care setting when the outcome may depend on timely management. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
